Introducing Super Logan, a Childhood Cancer Superhero!

“Super Logan” in the Batman costume in the middle.
Today, we’d like to introduce you to Logan, affectionately called “Super Logan” by his friends and family for his amazing, courageous fight against tremendous odds. On December 7, Logan and his family joined Hope 4 Heroes (ACCO’s Colorado-based Founding Hope Fund) and Rock Bottom Downtown Denver to participate in a public PJammin’ event organized by Colorado Rock Bottom Restaurants to raise awareness about childhood cancer. We would like to thank Logan and his family for taking the time to participate in this important event and for sharing their childhood cancer story with us.
Logan’s Story: Aggressive Stage Three Ependemoma (Brain Tumor)
Logan’s childhood cancer story began one evening in June, 2014 when he collapsed unconscious while walking to his parents’ bedroom. The five-year-old was rushed immediately to the local ER, where a CT scan showed that a large mass in his brain had hemorrhaged, causing paralysis on his left side. Logan was airlifted to a larger hospital, where his parents received the worst possible news: Logan had an inoperable brain tumor located inside his brainstem and he was unlikely to survive more than three days.
Logan’s parents, however, refused to accept this devastating diagnosis. They immediately sought a second opinion from surgeons at the Barrow Institute, part of the Phoenix Children’s Hospital, who believed that at least part of the tumor could be removed. Although the outcome was by no means guaranteed, surgeons felt that surgery could at least extend Logan’s life and give him a fighting chance. With nothing to lose, Logan was transferred to Phoenix Children’s Hospital for an eight-hour surgery.
In fact, the outcome was better than anyone could have imagined: Logan’s golf-ball-sized tumor was located entirely outside of the brainstem and the surgical team was able to remove it all, in its entirety. Logan’s family described the surgeon’s reaction when he told them the news as “giddy”, not a word one usually hears in these circumstances. Logan went into surgery hoping only that his life might be extended a little bit, but miraculously, came out cancer-free!
A Second Chance at Life, but A Very Long Road to Recovery
Yet despite this amazing outcome, Logan’s cancer journey was far from over. Although the tumor was gone, for now, Logan was unable to perform many basic functions that we take for granted every day, including talking, walking, and even swallowing. Moreover, he faced the very real possibility that the tumor, a fast-growing Ependemoma, would return without x-ray radiation therapy, a treatment as aggressive as the tumor and linked to significant long-term health risks and even secondary cancers.
Again, Logan’s family sought other options. So-called “traditional” X-ray radiation therapy is mostly commonly used as a post-surgical treatment for brain tumors like Logan’s, but is linked to severe side effects and even secondary cancers, especially in young children whose brains are still growing and developing. Instead, Logan’s parents took Logan to San Diego to undergo 6½ weeks of proton radiation therapy. The goal of proton radiation therapy is to more precisely target any remaining cancer cells, using pencil-beam scanning that carefully builds up the dose layer by layer exactly at the site of the tumor, hopefully limiting damage to surrounding healthy cells.
Thus far, Logan’s amazing “miracle” continues: his regular scans, although the source of extreme “scanxiety” so common for families fighting childhood cancer, have all come back clear, indicating that Logan is still cancer-free. But Logan still faces many, many challenges; “the past two years have been one trial after the next for our brave boy,” recounts Logan’s mother. Logan spent months in rehab after the surgery overcoming the paralysis caused by the tumor, re-learning to walk, talk, and even swallow. One therapist stated that Logan was one of the hardest swallowing cases she had ever seen and that her team honestly wasn’t sure if he would ever be able to swallow normally again.
The proton therapy has left its mark as well. He has been diagnosed with a vascular condition called Moyamoya and has suffered multiple strokes, including one that temporarily left him without sight. In March 2016, Logan underwent a second serious brain surgery. Most recently, abnormal weight gain has been linked to the development of central sleep apnea, a condition in which the brain no longer automatically commands breathing during sleep. Each day seems to bring new challenges to Logan and his family, but as his mother proudly notes, Logan never gives up: “Logan will always have battles to fight but we will be here and ready to stand strong next to him. He is an incredible boy and we are so proud to call him our son.
Thank you, Logan, for sharing your inspirational story with us and for showing us that it really is possible to fight, for showing us the true face of childhood cancer. You are a true Superhero!
About American Childhood Cancer Organization
American Childhood Cancer Organization (ACCO) is a non-profit charity dedicated to helping kids with cancer and their families navigate the difficult journey from cancer diagnosis through survivorship. Internationally, ACCO is the sole U.S. member of Childhood Cancer International (CCI), the largest patient-support organization for childhood cancer in the world. Here in the United States, ACCO promotes the critical importance of ensuring continued funding into new and better treatment protocols for childhood cancer. And most importantly, ACCO is focused on the children: developing and providing educational tools for children fighting cancer and their families, empowering them in their understanding of childhood cancer and the medical decisions they must make during this difficult journey. All of ACCO’s resources are available free of charge for families coping with childhood cancer.
For additional information about childhood cancer or on the ACCO, or to order resources for you or your child, please visit our website at www.acco.org , call 855.858.2226 or visit:
Want To Read American Childhood Cancer Organization On Your Phone? Click the NoteStream logo: 





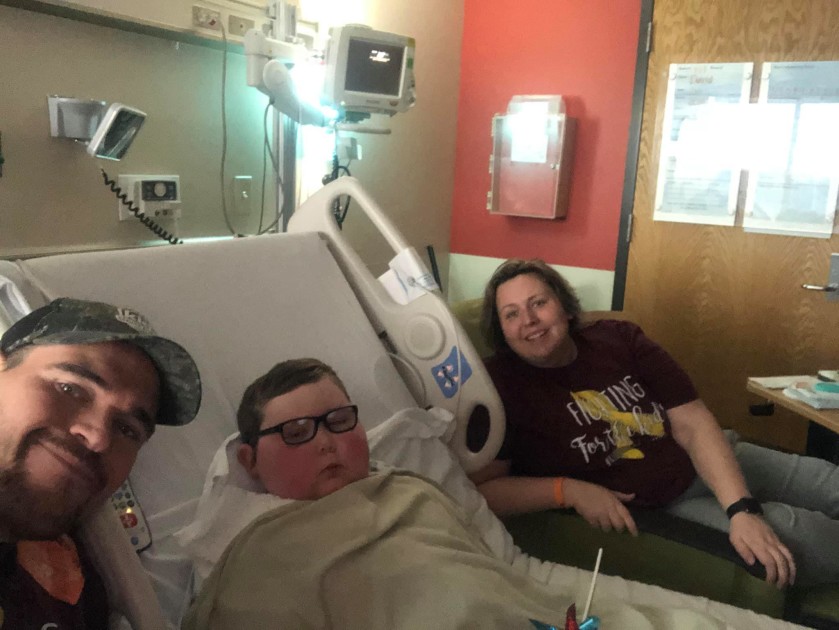 David was brought into the PICU almost immediately where they met the oncologist who advised David and Elizabeth about David Jr.’s condition, DIPG. Diffuse Intrinsic Pontine Glioma (DIPG) remains one of the deadliest forms of childhood cancer, with a long-term survival rate of less than 1%. After receiving the diagnosis from the oncologist, David’s parents decided they wanted to get a biopsy even though that was against the head of pediatric neurosurgery. They were advised that having the biopsy would not change the result and a cure didn’t currently exist.
David was brought into the PICU almost immediately where they met the oncologist who advised David and Elizabeth about David Jr.’s condition, DIPG. Diffuse Intrinsic Pontine Glioma (DIPG) remains one of the deadliest forms of childhood cancer, with a long-term survival rate of less than 1%. After receiving the diagnosis from the oncologist, David’s parents decided they wanted to get a biopsy even though that was against the head of pediatric neurosurgery. They were advised that having the biopsy would not change the result and a cure didn’t currently exist. swallow to talking like normal, walking normally and getting around with no assistance!
swallow to talking like normal, walking normally and getting around with no assistance!





 What are the key prognosis factors for childhood brain tumors?
What are the key prognosis factors for childhood brain tumors? When classed together in a single grouping, cancers in the brain and spinal cord are the second most common type of childhood cancer after leukemia. Brain and spinal cord tumors account for about 25% of all childhood cancer diagnoses, with more than 4,000 new cases diagnosed every year in the United States. In reality, however, it can be difficult to discuss “brain tumors” in general terms: oncologists recognize at least nine different sub-classifications of brain tumors in children, such as brain stem gliomas and ependymomas for example, with still more sub-groupings within those broad classifications.
When classed together in a single grouping, cancers in the brain and spinal cord are the second most common type of childhood cancer after leukemia. Brain and spinal cord tumors account for about 25% of all childhood cancer diagnoses, with more than 4,000 new cases diagnosed every year in the United States. In reality, however, it can be difficult to discuss “brain tumors” in general terms: oncologists recognize at least nine different sub-classifications of brain tumors in children, such as brain stem gliomas and ependymomas for example, with still more sub-groupings within those broad classifications. Generally speaking, “cancer” is a broad name for a condition in which cells in a particular part of the body begin to malfunction. They begin to grow, divide, and replicate more quickly than normal cells, and/or they do not die as normal when they are worn out or damaged. When these abnormal, or “cancerous”, cells originate in the brain or the spinal cord, they usually form a clump or a mass known as a tumor. As the cancerous cells continue to replicate, the tumor grows until it begins to cause damage to the brain and/or the spinal cord.
Generally speaking, “cancer” is a broad name for a condition in which cells in a particular part of the body begin to malfunction. They begin to grow, divide, and replicate more quickly than normal cells, and/or they do not die as normal when they are worn out or damaged. When these abnormal, or “cancerous”, cells originate in the brain or the spinal cord, they usually form a clump or a mass known as a tumor. As the cancerous cells continue to replicate, the tumor grows until it begins to cause damage to the brain and/or the spinal cord.
