Childhood Brain Tumor Cancer – Stages and Prognosis
When discussing childhood cancer, we often hear about the “stage” of the cancer. What does that mean, and is it relevant when discussing brain tumors in children? When oncologists first diagnose a case of cancer, part of the diagnosis usually involves an assessment of how and where the cancer has spread from the original point of growth. This assessment is known as “staging”. For many types of pediatric cancer, the “stage” of the cancer is an important factor in developing an appropriate treatment plan and determining the patient’s prognosis, or outlook.
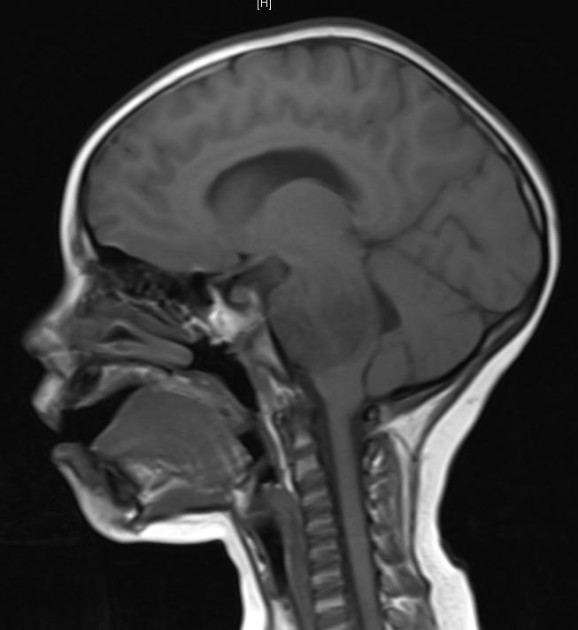 Is staging relevant for childhood brain tumors? In fact, this is one of the major differences between brain tumors and other types of cancers in children. Regardless of whether they are malignant (cancerous) or benign (non-cancerous), brain tumors in children rarely spread to other organs beyond the central nervous system (which includes the brain and the spinal cord). Therefore, oncologists do not utilize a formal staging system when diagnosing and treating brain cancers.
Is staging relevant for childhood brain tumors? In fact, this is one of the major differences between brain tumors and other types of cancers in children. Regardless of whether they are malignant (cancerous) or benign (non-cancerous), brain tumors in children rarely spread to other organs beyond the central nervous system (which includes the brain and the spinal cord). Therefore, oncologists do not utilize a formal staging system when diagnosing and treating brain cancers.
Yet although brain tumors do not generally present a threat to other organs of the body, both malignant and benign tumors can be extremely dangerous—and often life-threatening—as they interfere with the brain’s ability to function normally. As a brain tumor grows, it will press on, impede, or otherwise impair the healthy brain tissue nearby, depending on its precise location. Therefore, the location, size, and rate of growth are used to determining both treatment options and long-term prognosis, instead of more traditional “staging” used when diagnosing other types of cancers.
Prognosis Factors for Childhood Brain Tumors
Instead of staging, oncologists dealing with a diagnosis of a brain tumor will look at “prognosis factors” to help determine treatment options and to help assess each child’s potential for long-term survivorship. Some key prognosis factors include:
- The type of tumor: a brain tumor’s “type” is based on the type of cells from which the tumor began to grow. Some of the most common types of brain tumors in children include: gliomas (almost 50% of all brain tumors in children) such as glioblastomas, oligodendrogliomas, ependymomas, and brain stem gliomas; astrocytomas, and embryonal tumors (10-20% of all brain tumors in children) such as medulloblastomas.
- The tumor’s “grade”: A tumor is “graded” based on how quickly it is growing. Most oncologists use a four-level system of grading when dealing with brain tumors in children. Low grade tumors (grade I or grade II) usually grow relatively slowly and are less likely to invade or infiltrate adjacent healthy brain tissue. High grade tumors (grade III or grade IV) grow relatively quickly and are considered invasive. High grade tumors usually require a more aggressive treatment approach.
- The tumor’s location and size: The location and size of the tumor will greatly impact the symptoms the tumor causes, due to the specific functionality of the healthy brain tissue impacted by the growth of the tumor. Location and size will also determine treatment options; whether the tumor can be surgically removed, and how much of the tumor can be surgically removed, will greatly impact both treatment options and long-term prognosis.
Other prognosis factors for childhood brain tumors include:
- Whether the tumorous cells have specific gene mutations
- Whether the tumor has spread to other parts of the brain or spinal cord via the cerebrospinal fluid
- Whether tumorous cells have spread beyond the central nervous system
- The child’s age and functional abilities as impacted by the tumor
Just as every child is unique, so each cancer diagnosis is unique as well. If your child has been diagnosed with a brain tumor (whether benign or malignant), your child’s oncology team will ensure that you understand all of these prognosis factors as they relate to your child and his or her type of cancer. While the general guidelines contained here and in other similar literature are important, they are just that: only general guidelines. Only your child’s oncology team can determine your child’s key prognosis factors and their implications for long-term survivorship.
More about Childhood Brain Tumor Cancers:
- About Childhood Brain Tumor Cancer – Detection and Diagnosis
- Causes, Risk Factors, and Prevention of Childhood Brain Tumor Cancer
- What are the signs and symptoms of Childhood Brain Tumor Cancer?
- Childhood Brain Tumor Cancer Treatment
- Childhood Brain Tumor Cancer – Stages and Prognosis
- What is the expected life span of Childhood Brain Tumor Cancer?
- After Treatment – Living as a Childhood Brain Tumor Cancer Survivor
Learn More About the Different Types of Childhood Cancers:
- Childhood Brain Tumor Cancer (Brain Stem Tumors)
- Spinal Cord Tumor Cancer
- Childhood Neuroblastoma Cancers
- Childhood Hodgkin Lymphoma Cancers
- Non-Hodgkin Lymphoma Cancers
- Wilms tumor (Kidney Tumors)
- Rhabdomyosarcoma
- Retinoblastoma
- Bone cancer (including osteosarcoma and Ewing sarcoma)
- Leukemia Cancers: Acute lymphocytic (lymphoblastic) leukemia (ALL) Acute myelogenous leukemia (AML); Juvenile myelomonocytic leukemia (JMML)
- Hepatoblastoma (Liver Cancer)
- Rhabdoid Tumors
Together, we can make a difference.
Donate today because kids can’t fight cancer alone®.
About American Childhood Cancer Organization
The American Childhood Cancer Organization was founded in 1970 by parents of children and adolescents diagnosed with cancer. As the nation’s oldest and largest grassroots organization dedicated to childhood cancer, ACCO is committed to shaping policy, supporting research, raising awareness, and providing free educational resources to kids with cancer, survivors, and their families. Additionally, ACCO is the sole U.S. member of Childhood Cancer International (CCI) and has helped support more than half a million families over the past 50 years. Help make childhood cancer a national health priority because kids can’t fight cancer alone®.
For more information about how ACCO can help your family, call 855.858.2226 or visit:



 Meet Colton…
Meet Colton…
 According to Shannon, “radiation would only buy us time and there were trials we could participate in, but none were proven to save our child at this point.” During his treatment, Colton had multiple labs done, hospital stays, pneumonia, seizures and eventually lost his ability to walk, talk and swallow. He endured 30 rounds of radiation with a smile on his face. He also participated in a clinical trial for a year at Cincinnati Children’s Hospital.
According to Shannon, “radiation would only buy us time and there were trials we could participate in, but none were proven to save our child at this point.” During his treatment, Colton had multiple labs done, hospital stays, pneumonia, seizures and eventually lost his ability to walk, talk and swallow. He endured 30 rounds of radiation with a smile on his face. He also participated in a clinical trial for a year at Cincinnati Children’s Hospital. 
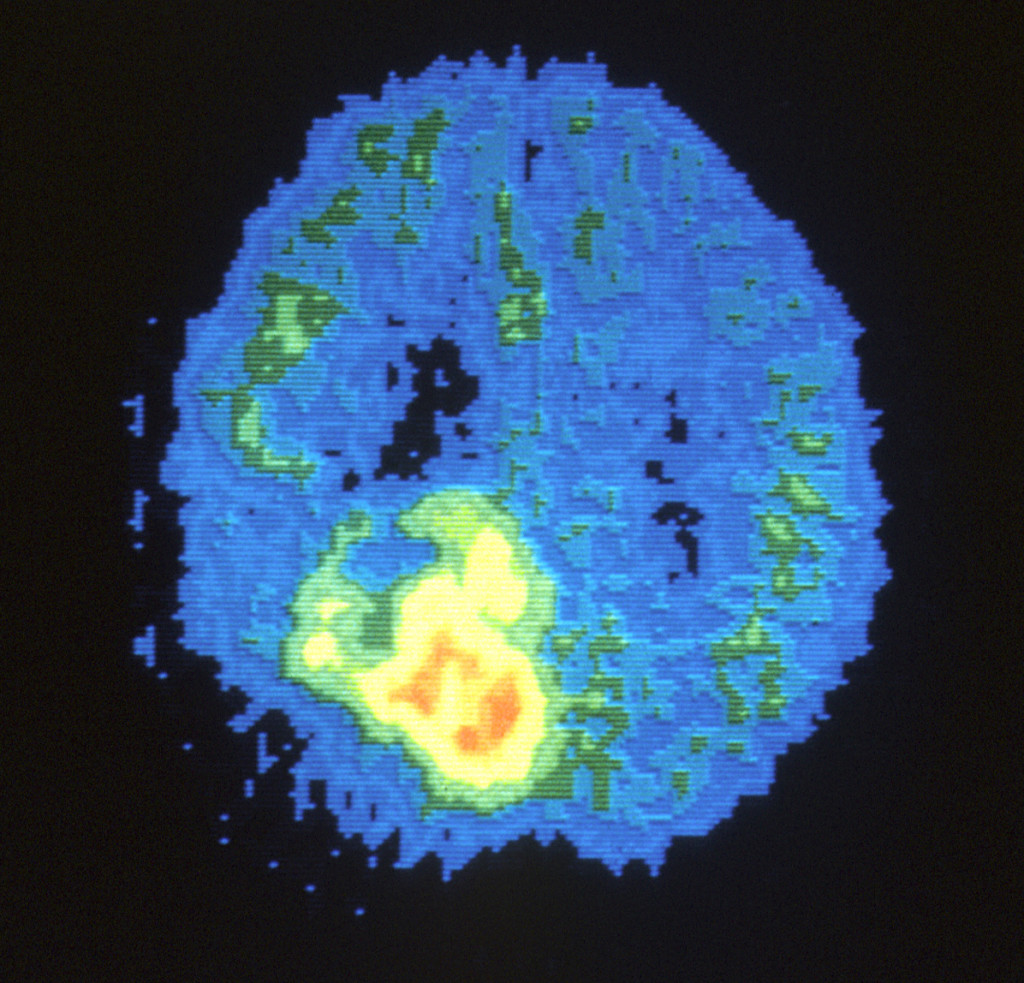 The brain is the “command center” for our entire central nervous system, yet despite its critical role in every aspect of human life, it is one of the most delicate organs in the entire body. Any abnormal growth, or tumor, in the brain—whether technically malignant (cancerous) or benign (non-cancerous)—can cause serious damage to the healthy brain tissue and significantly impact the body’s ability to function normally. Therefore, treating a brain tumor requires taking into consideration
The brain is the “command center” for our entire central nervous system, yet despite its critical role in every aspect of human life, it is one of the most delicate organs in the entire body. Any abnormal growth, or tumor, in the brain—whether technically malignant (cancerous) or benign (non-cancerous)—can cause serious damage to the healthy brain tissue and significantly impact the body’s ability to function normally. Therefore, treating a brain tumor requires taking into consideration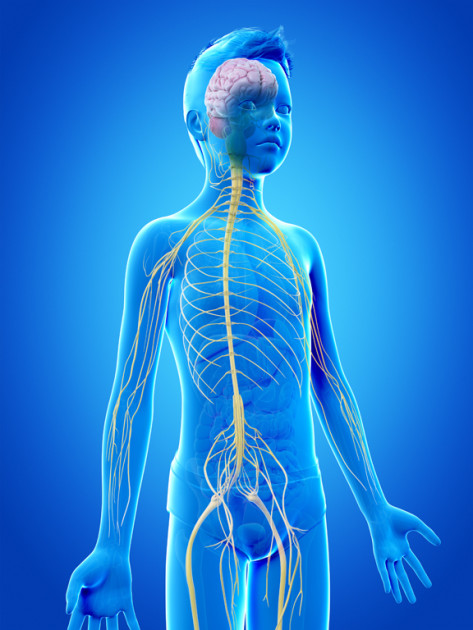 Taken together, the brain and the spinal cord make up what is known as the “central nervous system” (CNS). The CNS is responsible for our body’s most basic functions, like breathing, as well as higher order processing such as thinking and movement. So tumors that develop in a child’s central nervous system, whether the brain or spinal cord, can significantly impact the body’s normal functioning. Exactly what impact stems primary from where the tumor is located, how quickly it grows, and how much damage it causes to the healthy, but extremely delicate, tissues of the spinal cord and brain. Living as a survivor of a spinal cord tumor, whether benign or malignant, usually involves coping with symptoms that stem from (1) the growth of tumor itself and (2) the course of treatment needed to eliminate the tumor.
Taken together, the brain and the spinal cord make up what is known as the “central nervous system” (CNS). The CNS is responsible for our body’s most basic functions, like breathing, as well as higher order processing such as thinking and movement. So tumors that develop in a child’s central nervous system, whether the brain or spinal cord, can significantly impact the body’s normal functioning. Exactly what impact stems primary from where the tumor is located, how quickly it grows, and how much damage it causes to the healthy, but extremely delicate, tissues of the spinal cord and brain. Living as a survivor of a spinal cord tumor, whether benign or malignant, usually involves coping with symptoms that stem from (1) the growth of tumor itself and (2) the course of treatment needed to eliminate the tumor.
 When treatment began, Kyler could not comprehend what was going on, but now one year older, and Kyler can express his feelings about treatment and cope. Ashley said, “Over the last three months, Kyler has really began to cope with the disease. He has began to talk about his feelings and is understanding more and more. We try to explain things to him in a way he can understand.”
When treatment began, Kyler could not comprehend what was going on, but now one year older, and Kyler can express his feelings about treatment and cope. Ashley said, “Over the last three months, Kyler has really began to cope with the disease. He has began to talk about his feelings and is understanding more and more. We try to explain things to him in a way he can understand.”
 On May 3, 2018 Abby was diagnosed with a tumor in her brain. Debbie remembers, “We went into this room that felt like it was smaller than a cardboard box. That is when I heard the words, ‘Your daughter has a tumor in her brain. From where it is, I am thinking it is a cancer that children are known to get.
On May 3, 2018 Abby was diagnosed with a tumor in her brain. Debbie remembers, “We went into this room that felt like it was smaller than a cardboard box. That is when I heard the words, ‘Your daughter has a tumor in her brain. From where it is, I am thinking it is a cancer that children are known to get. 
 Radiation started just after Abby’s 7th birthday. After a few treatments, Abby’s scalp began to become sore so Debbie knew it was time to cut her hair shorter. Later, the radiation would take her hair. The harsh treatments made Abby see flashes of light and smell weird smells. These treatments required her to be face down and strapped to a board, which Abby did not like. Abby was able to ring the bell on July 19th after 30 rounds of radiation. On August 28, 2018, Abby started maintenance chemotherapy which will last until July 2019.
Radiation started just after Abby’s 7th birthday. After a few treatments, Abby’s scalp began to become sore so Debbie knew it was time to cut her hair shorter. Later, the radiation would take her hair. The harsh treatments made Abby see flashes of light and smell weird smells. These treatments required her to be face down and strapped to a board, which Abby did not like. Abby was able to ring the bell on July 19th after 30 rounds of radiation. On August 28, 2018, Abby started maintenance chemotherapy which will last until July 2019.
 Before beginning a discussion of general statistics relating to spinal cord tumors, it is important to note up front several key issues.
Before beginning a discussion of general statistics relating to spinal cord tumors, it is important to note up front several key issues. Meet Taylor, 16-year-old ambitious designer and entrepreneur. Taylor was determined to live life to the fullest, and wanted to be known as “a kid with cancer, never a cancer kid.” She didn’t want cancer to define her. Devastatingly, she passed away after a five year battle with cancer. Sue, her mother, said, “Taylor believed in life that all you need is love, and her memory is indelibly imprinted onto the hearts of everyone she left behind.”
Meet Taylor, 16-year-old ambitious designer and entrepreneur. Taylor was determined to live life to the fullest, and wanted to be known as “a kid with cancer, never a cancer kid.” She didn’t want cancer to define her. Devastatingly, she passed away after a five year battle with cancer. Sue, her mother, said, “Taylor believed in life that all you need is love, and her memory is indelibly imprinted onto the hearts of everyone she left behind.”
 In an excerpt from her book, “Paint Your Hair Blue, A Celebration of Life with Hope for Tomorrow in the Face of Pediatric Cancer” Sue writes: “Taylor’s life was not only about what she accomplished, but also about what she left behind. Her boundless optimism, even at the bleakest moments, and her zest for life, even as death neared, taught me more about love than I thought there was to know. Taylor believed in life that all you need is love, and her memory is indelibly imprinted onto the hearts of everyone she left behind.”
In an excerpt from her book, “Paint Your Hair Blue, A Celebration of Life with Hope for Tomorrow in the Face of Pediatric Cancer” Sue writes: “Taylor’s life was not only about what she accomplished, but also about what she left behind. Her boundless optimism, even at the bleakest moments, and her zest for life, even as death neared, taught me more about love than I thought there was to know. Taylor believed in life that all you need is love, and her memory is indelibly imprinted onto the hearts of everyone she left behind.”

 “It is hard to imagine what I felt. It was as if someone took my breath away and I found myself struggling just to breathe. As parents we don’t have the luxury of falling apart, and I quickly rallied to ask about the x-ray done in September when I was told that my son was constipated. They pulled the x-ray and the mass was in the same place that they misdiagnosed as constipation” remembers Patricia.
“It is hard to imagine what I felt. It was as if someone took my breath away and I found myself struggling just to breathe. As parents we don’t have the luxury of falling apart, and I quickly rallied to ask about the x-ray done in September when I was told that my son was constipated. They pulled the x-ray and the mass was in the same place that they misdiagnosed as constipation” remembers Patricia.