Treating Tumors of the Central Nervous System, including Spinal Cord Tumors
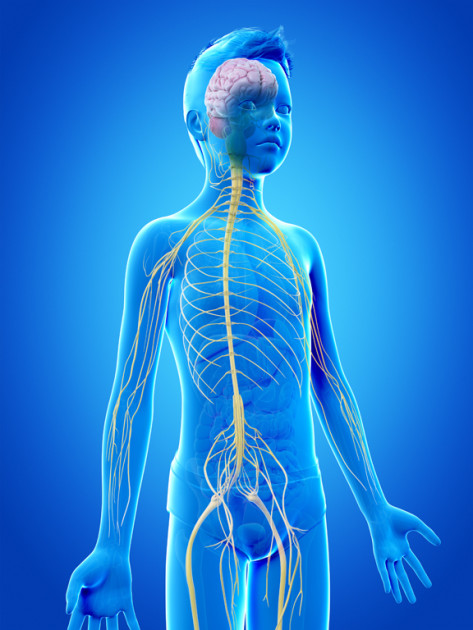 Taken together, the brain and the spinal cord make up what is known as the “central nervous system” (CNS). The CNS is responsible for our body’s most basic functions, like breathing, as well as higher order processing such as thinking and movement. So tumors that develop in a child’s central nervous system, whether the brain or spinal cord, can significantly impact the body’s normal functioning. Exactly what impact stems primary from where the tumor is located, how quickly it grows, and how much damage it causes to the healthy, but extremely delicate, tissues of the spinal cord and brain. Living as a survivor of a spinal cord tumor, whether benign or malignant, usually involves coping with symptoms that stem from (1) the growth of tumor itself and (2) the course of treatment needed to eliminate the tumor.
Taken together, the brain and the spinal cord make up what is known as the “central nervous system” (CNS). The CNS is responsible for our body’s most basic functions, like breathing, as well as higher order processing such as thinking and movement. So tumors that develop in a child’s central nervous system, whether the brain or spinal cord, can significantly impact the body’s normal functioning. Exactly what impact stems primary from where the tumor is located, how quickly it grows, and how much damage it causes to the healthy, but extremely delicate, tissues of the spinal cord and brain. Living as a survivor of a spinal cord tumor, whether benign or malignant, usually involves coping with symptoms that stem from (1) the growth of tumor itself and (2) the course of treatment needed to eliminate the tumor.
Therefore, before discussing either short- or long-term “late effects” resulting from a spinal cord tumor, a brief discussion of treatment options for spinal cord tumors makes sense. As with any course of cancer treatment, the goal of treatment is to remove as much of the tumor as possible and to prevent it from re-growing. Treatment will, as much as possible, seek to ameliorate or address symptoms caused by the position and the growth of the tumor in the first place.
- Surgery: If the spinal cord tumor is located in such a way that surgical removal is possible without causing further damage to healthy tissue, surgery to remove the tumor is usually the first course of treatment. The goal is total removal; however, in some cases, partial removal may be the only option.
- Radiation therapy: Radiation therapy is most commonly utilized to kill any remaining tumorous cells. Radiation may be the primary treatment if surgery is not possible due to the location of the tumor.
- Chemotherapy: Drug-based treatment—known as chemotherapy—is usually appropriate for targeting aggressive, fast-growing tumors, for the treatment of some tumors that are known to respond well to chemotherapy, and to treat children under the age of 3 for whom radiation is not usually considered appropriate.
However, for the majority of children diagnosed with a spinal cord tumor, a comprehensive treatment plan will involve some combination of all three approaches. Every treatment plan is unique to each specific child, depending on their unique health circumstances and type of tumor, in order to maximize their chances of long-term survival while simultaneously minimizing the risk of short- and long-term health problems.
Living as a Survivor of Childhood Spinal Cord Cancer
Health problems resulting from either the growth of the tumor itself or from the powerful treatment required to eliminate the tumor are usually called “late effects” and can manifest at any point in a child’s development, even years down the road. Unfortunately, children are especially prone to problematic “late effects” because their CNS is growing and developing so much more actively than an adult’s.
Throughout treatment and afterwards, your child’s oncology team will assess potential damage to the spinal cord with the goal of recommending specific follow-up treatment(s) to mitigate any side effects. Coping with late effects often involves a variety of different medical specialists, particularly physical and occupational therapists who can help address concerns relating to movement, which is often the most impacted by spinal cord tumors. Psychologists and learning specialists may also be useful for coping with the emotional effects of a cancer diagnosis and treatment.
Two critical—and too often overlooked—elements of living as a spinal cord tumor survivor are:
- Faithfully sticking to the schedule of follow-up exams and tests as laid out by your child’s oncology team. While often stressful, these visits are necessary to monitor signs that the tumor is re-developing, or to monitor for so-called secondary cancers which may result from radiation and/or chemotherapy treatment.
- Maintaining well-organized records of your child’s cancer treatment. These records will ensure that new doctors throughout your child’s life have a comprehensive understanding of your child’s medical history. This will help successfully address any late effects or other health concerns that may arise, whether or not related to the spinal cord tumor.
More about Childhood Spinal Cord Tumor Cancers:
- About Childhood Spinal Cord Tumor Cancer – Detection and Diagnosis
- Causes, Risk Factors, and Prevention of Childhood Spinal Cord Tumor Cancer
- What are the signs and symptoms of Childhood Spinal Cord Tumor Cancer?
- Spinal Cord Tumor Cancer Treatment
- Spinal Cord Tumor Cancer – Stages and Prognosis
- What is the expected life span of Childhood Spinal Cord Tumor Cancer?
- After Treatment – Living as a Childhood Spinal Cord Tumor Cancer Survivor
Learn More About the Different Types of Childhood Cancers:
- Childhood Brain Tumor Cancer (Brain Stem Tumors)
- Spinal Cord Tumor Cancer
- Childhood Neuroblastoma Cancers
- Childhood Hodgkin Lymphoma Cancers
- Non-Hodgkin Lymphoma Cancers
- Wilms tumor (Kidney Tumors)
- Rhabdomyosarcoma
- Retinoblastoma
- Bone cancer (including osteosarcoma and Ewing sarcoma)
- Leukemia Cancers: Acute lymphocytic (lymphoblastic) leukemia (ALL) Acute myelogenous leukemia (AML); Juvenile myelomonocytic leukemia (JMML)
- Hepatoblastoma (Liver Cancer)
- Rhabdoid Tumors
Together, we can make a difference.
Donate today because kids can’t fight cancer alone®.
About American Childhood Cancer Organization
The American Childhood Cancer Organization was founded in 1970 by parents of children and adolescents diagnosed with cancer. As the nation’s oldest and largest grassroots organization dedicated to childhood cancer, ACCO is committed to shaping policy, supporting research, raising awareness, and providing free educational resources to kids with cancer, survivors, and their families. Additionally, ACCO is the sole U.S. member of Childhood Cancer International (CCI) and has helped support more than half a million families over the past 50 years. Help make childhood cancer a national health priority because kids can’t fight cancer alone®.
For more information about how ACCO can help your family, call 855.858.2226 or visit:


