The American Childhood Cancer Organization is a key leader in providing a voice within the halls of Congress for children and families affected by a childhood cancer diagnosis. We believe the urgent cries of children with cancer have been silenced by hospital walls for too long. Each child is special and should be valued, not treated as a faceless statistic. We believe personal stories matter – when shared with elected officials they are our most powerful weapon in the fight against childhood cancer. With the recent implementation of a new grassroots advocacy software system called Voter Voice, we’ve made it easier and faster than ever for our advocates to take action to contact elected officials at the state and federal level from home, or even the hospital.
In the past year, ACCO gave children battling cancer as well as childhood cancer survivors a voice as a multitude of health insurance policies were debated that directly jeopardized their lives. Our advocacy emphasized the importance of maintaining the requirement for any proposal to cover essential health benefits while prohibiting annual or lifetime caps on coverage. We also spoke out against allowing states flexibility to limit or even exclude coverage for children with cancer because of pre-existing conditions. Additionally, we stood up for the one-third of all children diagnosed with cancer who depend on Medicaid to provide life-saving treatments by opposing drastic cuts in funding.
In the past year we’ve also empowered advocates to be a part of the passing the RACE for Children Act – a revolutionary piece of drug development policy that will promote access to the latest cancer drugs being developed for adults that have a common molecular pathway in pediatric cancer types. This will help ensure children have access to new cancer treatments too. Currently stakeholders are participating in public meetings to determine the list of molecular targets to be included by the Federal Drug Administration as a result of the Race for Children Act.
We are very excited that on June 5, 2018 – after three years and thousands of you took action – the Childhood Cancer STAR (Survivorship, Treatment, Access, Research) Act was signed into law! The most comprehensive childhood cancer legislation ever to be considered by Congress, this bill will increase overall pediatric cancer research funding at the National Institute for Health as well as expand research about the complicated issues of long-term survivorship; improve data collection for better outcomes utilizing shared information; and ensure childhood cancer has improved representation on the National Cancer Advisory Board.
Now the STAR Act needs to be fully funded each year for the next five years. Visit our Take Action center to stay up to date on our progress and take further action to keep the STAR Act moving.
Finally, we are proud to serve as a key member of the Alliance for Childhood Cancer, a collaboration of over 30 national advocacy groups uniting together towards one key purpose, ending the devastation of childhood cancer. As part of the Alliance, ACCO serves as a part of the Policy Workgroup to guide overall decision-making for legislation, policy, and initiatives the collective organizations will support. In addition to legislation, as a part of this collaborative the ACCO joins other members in advocating for increased funding for childhood cancer research in the National Institute of Health and the National Cancer Institute.


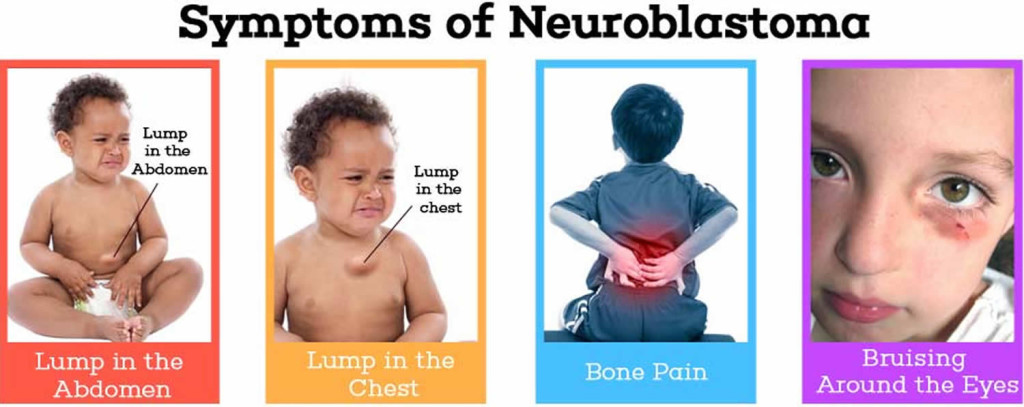 In many cases, symptoms of neuroblastoma are caused by a tumor, or mass of cancerous cells, that becomes visible through the skin or begins to press on other organs of the body. The location of the primary tumor will impact the specific symptoms the child is experiencing. For instance:
In many cases, symptoms of neuroblastoma are caused by a tumor, or mass of cancerous cells, that becomes visible through the skin or begins to press on other organs of the body. The location of the primary tumor will impact the specific symptoms the child is experiencing. For instance: More about Childhood Neuroblastoma Cancers:
More about Childhood Neuroblastoma Cancers:



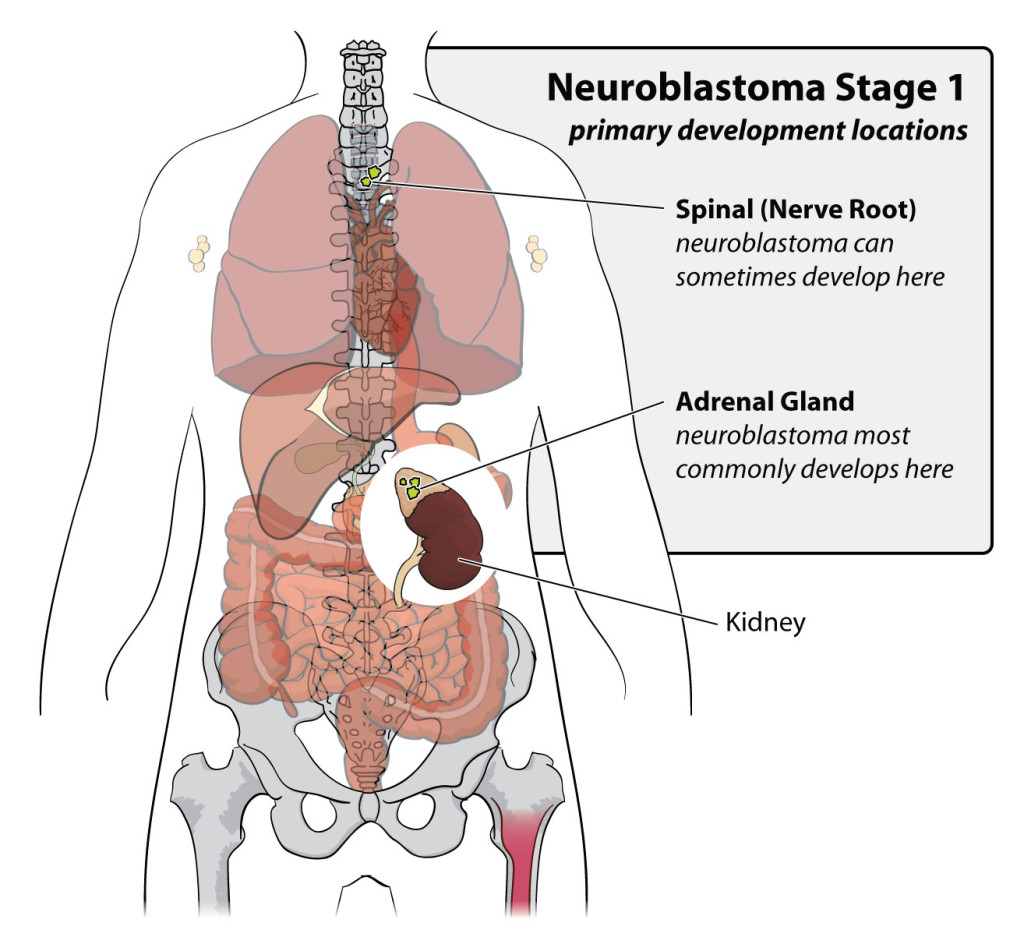 Neuroblastoma is caused by the abnormal development of immature nerve cells known as neuroblasts. As a fetus develops, most neuroblasts grow and eventually become mature nerve cells either before birth or in the first few months after birth. However, in some cases, neuroblasts do not develop correctly. Instead of becoming mature nerve cells, they continue to grow and divide. In some cases, these abnormal neuroblasts simply die off; however, in some rare cases, they develop into tumors or neuroblastoma.
Neuroblastoma is caused by the abnormal development of immature nerve cells known as neuroblasts. As a fetus develops, most neuroblasts grow and eventually become mature nerve cells either before birth or in the first few months after birth. However, in some cases, neuroblasts do not develop correctly. Instead of becoming mature nerve cells, they continue to grow and divide. In some cases, these abnormal neuroblasts simply die off; however, in some rare cases, they develop into tumors or neuroblastoma. Clinical trials are a part of long-term research studies designed to develop and test potential new treatment options for cancer and other illnesses. When a team of physicians and/or scientists believes they have developed a potentially effective new treatment, they will first study the treatment in the lab, and then potentially test it on animals. If the new treatment shows promise, it may be tested in people through a multi-phase clinical trial. This is an important step in determining whether a new treatment gets government approval and can be incorporated into existing treatment protocols. Clinical trials are a critical part of the on-going fight to develop new and better treatment options for cancers, especially childhood cancers.
Clinical trials are a part of long-term research studies designed to develop and test potential new treatment options for cancer and other illnesses. When a team of physicians and/or scientists believes they have developed a potentially effective new treatment, they will first study the treatment in the lab, and then potentially test it on animals. If the new treatment shows promise, it may be tested in people through a multi-phase clinical trial. This is an important step in determining whether a new treatment gets government approval and can be incorporated into existing treatment protocols. Clinical trials are a critical part of the on-going fight to develop new and better treatment options for cancers, especially childhood cancers. Neuroblastoma is a type of childhood cancer that develops in immature nerve cells within the sympathetic nervous system. Part of the autonomic nervous system (which controls bodily functions we do not consciously control, such as breathing and heart rate), the sympathetic nervous system is made up of nerve fibers that run parallel to the spinal cord, ganglia (clusters of nerve cells) found along the nerve fibers, and nerve-like cells located in the adrenal glands. Neuroblastoma begins to grow in the very early forms of nerve cells as they develop in the embryo or fetus.
Neuroblastoma is a type of childhood cancer that develops in immature nerve cells within the sympathetic nervous system. Part of the autonomic nervous system (which controls bodily functions we do not consciously control, such as breathing and heart rate), the sympathetic nervous system is made up of nerve fibers that run parallel to the spinal cord, ganglia (clusters of nerve cells) found along the nerve fibers, and nerve-like cells located in the adrenal glands. Neuroblastoma begins to grow in the very early forms of nerve cells as they develop in the embryo or fetus. On average in the United States each year, there are more than 4,000 new diagnoses of
On average in the United States each year, there are more than 4,000 new diagnoses of  The brain and central nervous system control every aspect of our body, from its most basic functions such as breathing to significantly more complex functions such as movement and balance. The brain even controls personality and social interactions. So tumors located in the brain or spinal cord, whether they are benign or malignant, can significant impact how our body functions depending on where they grow and how much damage they inflict on healthy brain tissue. Survivorship issues for children with
The brain and central nervous system control every aspect of our body, from its most basic functions such as breathing to significantly more complex functions such as movement and balance. The brain even controls personality and social interactions. So tumors located in the brain or spinal cord, whether they are benign or malignant, can significant impact how our body functions depending on where they grow and how much damage they inflict on healthy brain tissue. Survivorship issues for children with  WASHINGTON, D.C. – APRIL 23rd – 24th, 2018
WASHINGTON, D.C. – APRIL 23rd – 24th, 2018