How is Childhood Hodgkin Lymphoma Detected?
As with most types of childhood cancer, there is no method of early detection for childhood Hodgkin lymphoma. Childhood Hodgkin lymphoma does cause detectable symptoms; however, the symptoms are usually general and vague, and may in fact be caused by a variety of routine childhood complaints.
Symptoms of childhood Hodgkin lymphoma may include:
- Fatigue
- Unexplained fever
- Unexplained and significantly weight loss (defined as at least 10% of body weight within 6 months of diagnosis)
- Night sweats
- Itchy skin
The most common symptom of childhood Hodgkin lymphoma is one or more swollen lymph node(s) in the neck, armpit, chest, and/or groin area. As with the other symptoms listed above, however, a swollen lymph node may—and very often does—have other causes than childhood Hodgkin lymphoma. Swollen lymph nodes are usually caused by infection because the lymph nodes are responsible for helping the body clear the blood of foreign viruses and bacteria. Swollen lymph nodes caused by infection are usually uncomfortable and painful to the touch, and can be treated with antibiotics.
If the lump caused by the swollen lymph node does not diminish over time, does not respond to antibiotics, and/or is not uncomfortable or painful, or if your child has a swollen lymph node and one or more of the symptoms noted above, your child’s pediatrician may suspect the presence of Hodgkin lymphoma and suggest additional testing.
How is Childhood Hodgkin Lymphoma Diagnosed?
Once infection has been ruled out as the cause of any swollen lymph nodes, the next step in determining whether your child has childhood Hodgkin lymphoma is to perform a biopsy on the affected lymph node tissue. A biopsy involves removing some or all of the affected tissue and examining it under a microscope to detect the presence of cancerous cells. Depending on the location of the lump, the biopsy can be performed under local anesthesia (for lumps located near the surface of the skin) or under general anesthesia (for lumps located deeper inside the abdomen or chest).
 There are two different types of biopsies that can potentially be used to diagnose childhood Hodgkin lymphoma. The preferred method is an excisional or incisional biopsy, because in most cases it involves removal of enough tissue to diagnose the exact type of Hodgkin lymphoma as well to help in staging. In an excisional biopsy, the entire lymph node is removed. During an incisional biopsy, a small piece of the swollen lymph node is removed.
There are two different types of biopsies that can potentially be used to diagnose childhood Hodgkin lymphoma. The preferred method is an excisional or incisional biopsy, because in most cases it involves removal of enough tissue to diagnose the exact type of Hodgkin lymphoma as well to help in staging. In an excisional biopsy, the entire lymph node is removed. During an incisional biopsy, a small piece of the swollen lymph node is removed.
A needle biopsy is less invasive than an excisional or incisional biopsy, but is usually not preferred as it may not provide sufficient tissue for an accurate diagnosis. A fine needle aspiration biopsy utilizes an extremely small, hollow needle to remove a small amount of fluid and tissue, while a core needle biopsy uses a larger needle and removes a slightly larger amount of fluid and tissue.
Once childhood Hodgkin lymphoma has definitely been diagnosed with a biopsy, your child may have to undergo additional testing to determine the specific type of Hodgkin lymphoma and the stage of the disease (how far it has progressed). This information will help determine the recommend course of treatment. Additional tests may include:
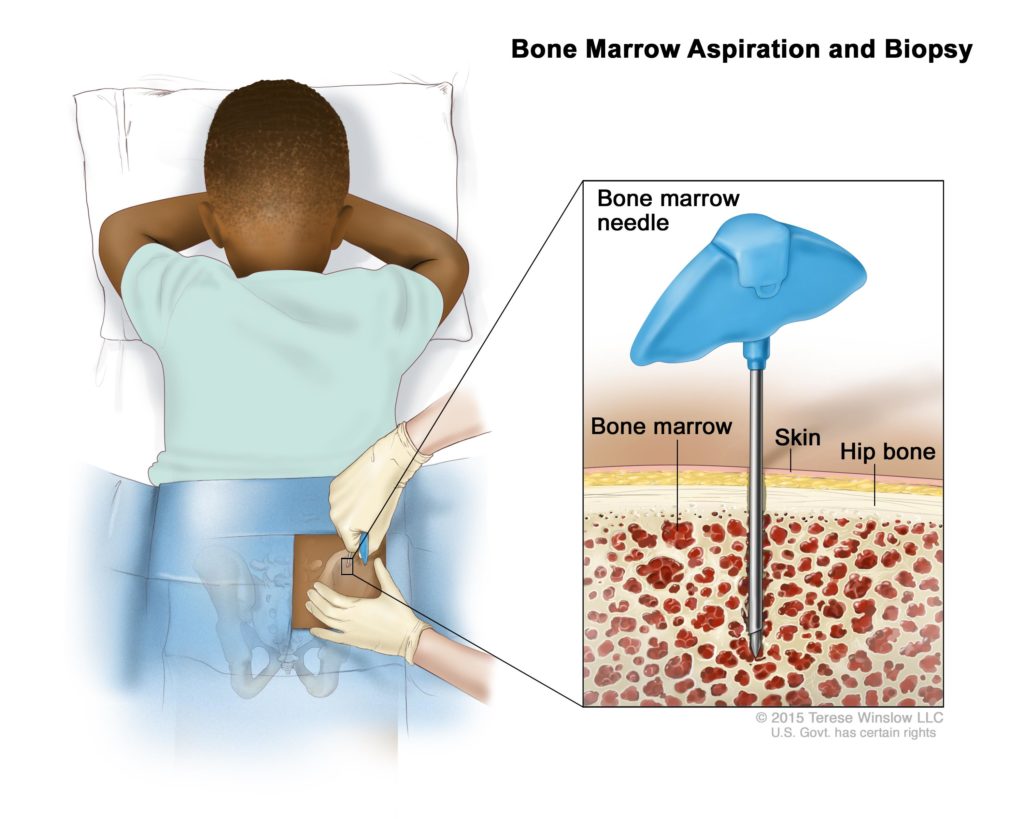
- Bone marrow aspiration: a sample of bone marrow is removed from the inside of the pelvic bone (usually); in some cases, the test may involve removing a small sample of bone as well. A biopsy of the bone and/or marrow will indicate whether cancerous cells have spread to the marrow.
- Immunohistochemistry: this laboratory test determines whether certain proteins are present on the cancerous cells, in order to determine the exact type of Hodgkin lymphoma, for instance, or to diagnose non-Hodgkin lymphoma or another disease entirely.
- Imaging tests, such as chest x-ray, CT scan, and/or PET scan: While not generally used during diagnoses, imaging tests can be used to determine the stage of the disease and whether treatment is working. In some cases, imaging tests may be used to detect and/or biopsy enlarged lymph nodes not readily apparent with an easily visible lump, such as those located in the chest.
More about Childhood Hodgkin Lymphoma Cancers:
- About Childhood Hodgkin Lymphoma Cancer – Detection and Diagnosis
- Causes, Risk Factors, and Prevention of Childhood Hodgkin Lymphoma Cancer
- What are the signs and symptoms of Childhood Hodgkin Lymphoma Cancer?
- Childhood Hodgkin Lymphoma Cancer Treatment
- Childhood Hodgkin Lymphoma Cancer – Stages and Prognosis
- What is the expected life span of Childhood Hodgkin Lymphoma Cancer?
- After Treatment – Living as a Childhood Hodgkin Lymphoma Cancer Survivor
Learn More About the Different Types of Childhood Cancers:
- Childhood Brain Tumor Cancer (Brain Stem Tumors)
- Spinal Cord Tumor Cancer
- Childhood Neuroblastoma Cancers
- Childhood Hodgkin Lymphoma Cancers
- Non-Hodgkin Lymphoma Cancers
- Wilms tumor (Kidney Tumors)
- Rhabdomyosarcoma
- Retinoblastoma
- Bone cancer (including osteosarcoma and Ewing sarcoma)
- Leukemia Cancers: Acute lymphocytic (lymphoblastic) leukemia (ALL) Acute myelogenous leukemia (AML); Juvenile myelomonocytic leukemia (JMML)
- Hepatoblastoma (Liver Cancer)
- Rhabdoid Tumors
About American Childhood Cancer Organization
American Childhood Cancer Organization (ACCO) is a non-profit charity dedicated to helping kids with cancer and their families navigate the difficult journey from cancer diagnosis through survivorship. Internationally, ACCO is the sole U.S. member of Childhood Cancer International (CCI), the largest patient-support organization for childhood cancer in the world. Here in the United States, ACCO promotes the critical importance of ensuring continued funding into new and better treatment protocols for childhood cancer. And most importantly, ACCO is focused on the children: developing and providing educational tools for children fighting cancer and their families, empowering them in their understanding of childhood cancer and the medical decisions they must make during this difficult journey. All of ACCO’s resources are available free of charge for families coping with childhood cancer.
For additional information about childhood cancer or on the ACCO, or to order resources for you or your child, please visit our website at www.acco.org , call 855.858.2226 or visit:

