Meet Grace – a sweet and spirited 9 year old and one of our Ambassadors for Childhood Cancer Awareness Month. Grace is a generous and giving individual with a passion to help others and brighten their days. She is strong and courageous, even when things might not be easy.

Grace is a typical 9-year-old, she loves gymnastics, softball, riding her bike, reading, painting and swimming. She also loves playing with her friends. This little warrior exudes good vibes and positive energy 24/7. For every birthday, Grace requested that in lieu of gifts, money should be donated to St. Jude Children’s Research Hospital. Little did she know, she might be the recipient of services from them in the future.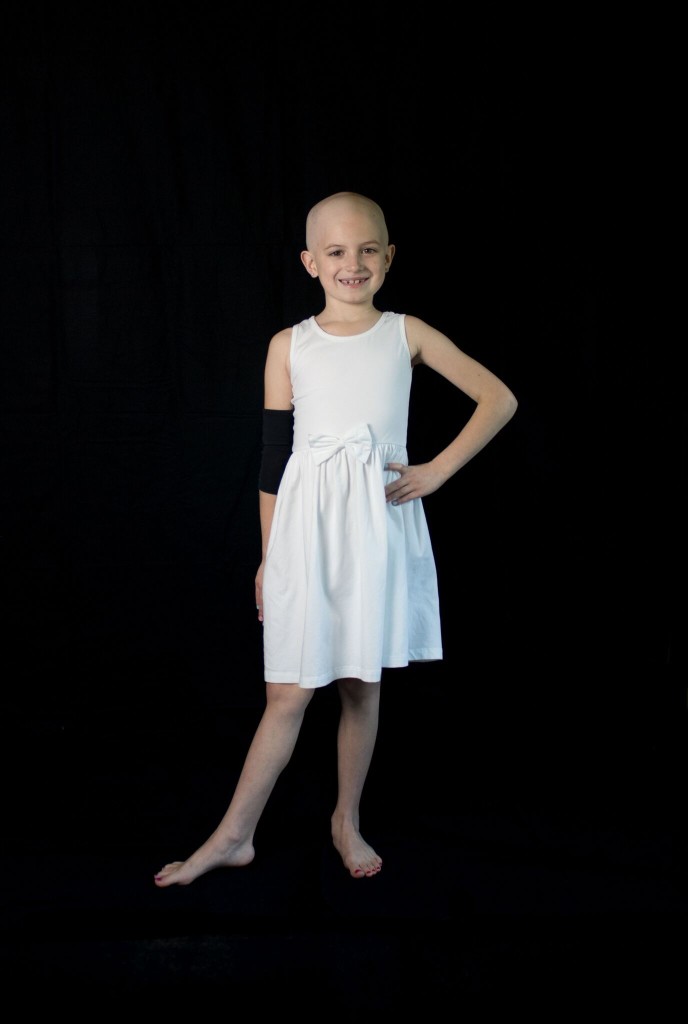
Aubrey, Grace’s mom, said “Grace was always the tallest in her class, and then one day she wasn’t. She was drinking a lot of water, so it warranted a closer look. A proactive pediatrician and endocrinologist ordered a brain MRI which resulted in the detection of a mass around Grace’s pituitary gland dangerously close to her optic nerves.” The initial tumor was detected on April 9, 2018 and over the next few weeks, Grace endured scans at the neurosurgeons office. After discussing things with the doctor at length, Grace decided she wanted to be a doctor. She had more tests, scans and plenty of needles and laid still for each of them. She got through all of the tests by listening to songs on her playlist and smiling as best she could. Grace even comforted her queasy mother and support team.
Grace was diagnosed with Germinoma brain cancer, a germ cell brain tumor, on May 2, 2018. Her aggressive treatment began on May 9, 2018 and she just finished the radiation portion of treatment. As of today, there is no evidence of a tumor and Grace will undergo blood tests, MRIs and spinal taps for the next few months to monitor the success of the chemo.
 Grace loves to be crafty; she made a sign for the children to sign and date which says “Last Day of Chemo.” Throughout her treatment, she decided to paint pictures to brighten the nurses and the children’s days. When losing her hair became a reality, Grace decided to throw a party and shave her head. Grace’s brother and her best friend joined her in shaving their heads as well.
Grace loves to be crafty; she made a sign for the children to sign and date which says “Last Day of Chemo.” Throughout her treatment, she decided to paint pictures to brighten the nurses and the children’s days. When losing her hair became a reality, Grace decided to throw a party and shave her head. Grace’s brother and her best friend joined her in shaving their heads as well.
According to Grace’s mom, “The hardest thing in the process has been missing school. She is one of ‘those kids’ that is passionate about being in school. She video conferences in as much as she can and keeps up on all her projects, even the ones for her future’s gifted program. She rallied a huge team for a fundraiser walk for her hospital and came in second place overall for fundraising. She was the first place for largest team.”
Grace is determined to help people and is currently making a plan of how she will continue helping other kids with cancer. She enjoys ta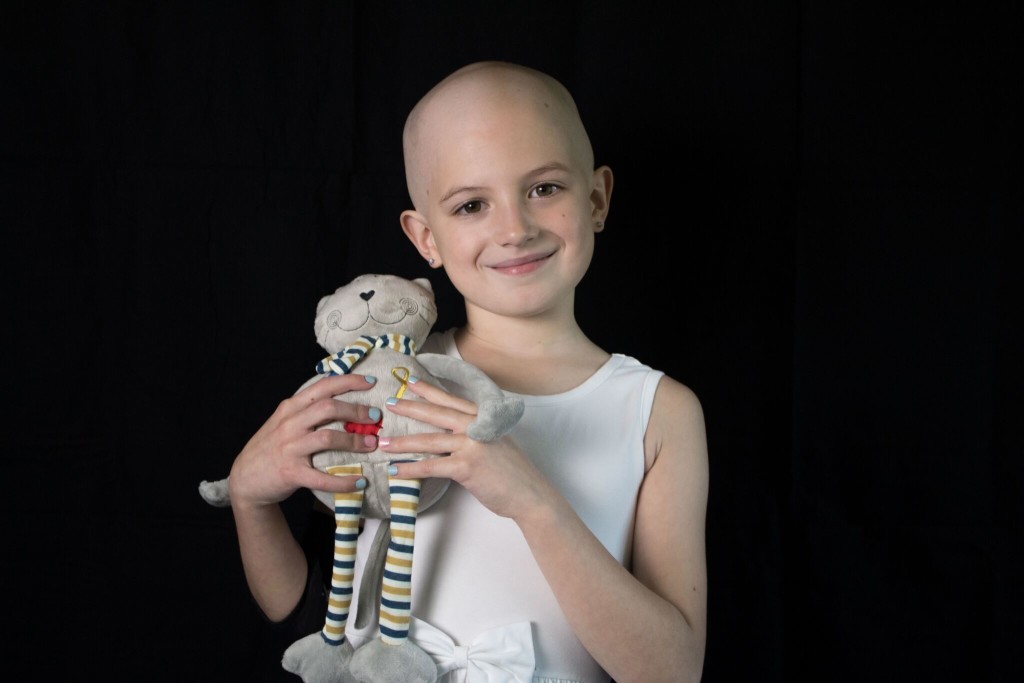 lking to people about this part of her journey and is focused on helping others. Grace plans on learning more about oncology. She is excited for the future and can’t wait for her hair to start growing back!
lking to people about this part of her journey and is focused on helping others. Grace plans on learning more about oncology. She is excited for the future and can’t wait for her hair to start growing back!
*Special thanks to Barbara Zobian and the Candlelighters NYC*



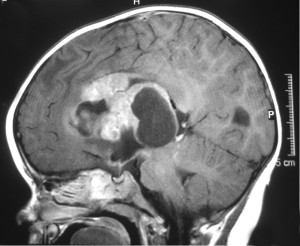 Any time a child is diagnosed with a brain tumor or other type of cancer, the most obvious question many parents ask is “why”. What caused this child to develop a brain tumor? Unfortunately, there is no easy answer to this question. Scientists now believe that the vast majority of brain tumors in children are the result of random gene mutations but have no satisfying answer as to why a particular gene mutation occurred or why it led to the growth of a brain tumor.
Any time a child is diagnosed with a brain tumor or other type of cancer, the most obvious question many parents ask is “why”. What caused this child to develop a brain tumor? Unfortunately, there is no easy answer to this question. Scientists now believe that the vast majority of brain tumors in children are the result of random gene mutations but have no satisfying answer as to why a particular gene mutation occurred or why it led to the growth of a brain tumor. After leukemia, brain tumors (including spinal cord tumors) are the second-most common type of cancer in children, accounting for about 25% of all childhood cancer diagnoses. Brain tumors begin within the delicate and complicated tissues of the brain or the cerebrospinal fluid (as well as the spinal cord or central nervous system, as these tumors are usually classed with brain tumors in children). When dealing with brain tumors in children, oncologists rarely differentiate between benign (non-cancerous) or malignant (cancerous) tumors; all tumors in the brain can be life-threatening whether technically cancerous or not. Instead, oncologists usually focus on how fast the tumor is growing, how quickly or easily it may spread throughout the brain or spinal cord, and how easy the tumor is to remove completely.
After leukemia, brain tumors (including spinal cord tumors) are the second-most common type of cancer in children, accounting for about 25% of all childhood cancer diagnoses. Brain tumors begin within the delicate and complicated tissues of the brain or the cerebrospinal fluid (as well as the spinal cord or central nervous system, as these tumors are usually classed with brain tumors in children). When dealing with brain tumors in children, oncologists rarely differentiate between benign (non-cancerous) or malignant (cancerous) tumors; all tumors in the brain can be life-threatening whether technically cancerous or not. Instead, oncologists usually focus on how fast the tumor is growing, how quickly or easily it may spread throughout the brain or spinal cord, and how easy the tumor is to remove completely.