Childhood Brain and Spinal Cord Tumors: A Brief Introduction
 When grouped together in a single classification, cancers in the brain and spinal cord are the second most common form of cancer in children after childhood leukemia, with more than 4,000 new diagnoses every year. However, it is important to recognize that this is a very broad classification: in fact, there are many different types of brain and spinal cord cancers, each of which can cause different symptoms and each of which may require a unique treatment approach. It is also important to note at the outset of any discussion about cancers of the brain and spinal cord that, unlike in other areas of the body, oncologists do not differentiate between benign (non-cancerous) and malignant (cancerous) tumors in the central nervous system. Both types of tumors can be life-threatening if not treated. For this reason, oncologists usually refer to “brain tumors” instead of “brain cancers”.
When grouped together in a single classification, cancers in the brain and spinal cord are the second most common form of cancer in children after childhood leukemia, with more than 4,000 new diagnoses every year. However, it is important to recognize that this is a very broad classification: in fact, there are many different types of brain and spinal cord cancers, each of which can cause different symptoms and each of which may require a unique treatment approach. It is also important to note at the outset of any discussion about cancers of the brain and spinal cord that, unlike in other areas of the body, oncologists do not differentiate between benign (non-cancerous) and malignant (cancerous) tumors in the central nervous system. Both types of tumors can be life-threatening if not treated. For this reason, oncologists usually refer to “brain tumors” instead of “brain cancers”.
Childhood Brain and Spinal Cord Tumors: Detection Through Common Signs and Symptoms
As with all childhood cancers, there is no “early detection” screening process for tumors of the central nervous system. Diagnosis usually comes after parents begin to observe unusual medical symptoms. Most symptoms of brain and spinal cord tumors are caused by the tumor raising the pressure inside the brain (known as intracranial pressure). The increase in intracranial pressure can lead to symptoms such as:
- Headaches
- Nausea and vomiting
- Crossed eyes and/or blurred vision
- Balance problems
- Behavioral changes
- Seizures
- Drowsiness, potentially leading to coma
Of course, most of these symptoms are extremely common and are only rarely caused by a tumor. However, if symptoms continue over time or worsen, or in the case of seizures begin very suddenly, your pediatrician may recommend testing to properly diagnose the cause of the medical issue as quickly as possible.
Because the central nervous system controls the function of the entire body, the location of the tumor within the brain or spinal column may cause different types of symptoms:
- Tumors in the cerebrum (large, outer part of the brain) can cause symptoms relating to the specific function controlled by the area of the cerebrum affected by the growth of the tumor, such as:
- Tumors in the area of the cerebrum responsible for movement can lead to weakness or numbness in a specific part of the body, usually only on one side
- Tumors in the area of the cerebrum responsible for language can cause speech or comprehension problems
- Tumors at the front of the cerebrum can lead to issues with thinking, personality, and language skills
- Tumors at the back of the cerebrum or near cranial nerves can cause issues with vision
- Tumors in the cerebellum can cause symptoms relating to walking or other normal body functions
- Tumors in the basal ganglia can cause unusual or abnormal body positions or movements
- Tumors in cranial nerves (not those in the cerebrum) may cause loss of hearing, balance issues, weakness of facial muscles, or potentially trouble with swallowing
- Tumors in the spinal cord may cause numbness, weakness, lack of coordination, and even bladder and/or bowel concerns
Childhood Brain and Spinal Cord Tumors: Diagnosis
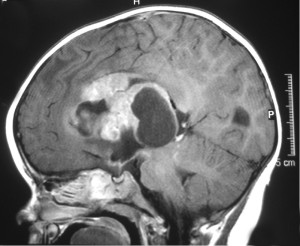
In most cases, the first step in diagnosing a brain or spinal column is an imaging test, most likely an MRI (magnetic resonance imaging). An MRI is able to create detailed images of the brain using a combination of radio waves and strong magnets; moreover, it does not involve the use of radiation, which can be extremely damaging to the brain tissue of young children. While not painful or physically invasive, an MRI can be a difficult test for some children. It can take a long time and often requires the patient to stay still in a confining tube for an extended period. Some children may require sedation or medication to help them relax in order to make this test less stressful.
Should the MRI or other imaging scan reveal a tumor, the next step is, when possible, to conduct a biopsy, in which some or all of the tumorous tissue is removed from the body and examined under a microscope. A biopsy may be done simultaneously with surgery to remove the entire tumor, or it may be done as a stand-alone procedure in order to determine next steps in treatment. In some cases, usually due to the location of the tumor in a sensitive or dangerous area of the brain or spinal cord, a physical biopsy may not be possible and diagnosis must be made on the basis of imaging alone.
Specific types of biopsies include:
- Stereotactic needle biopsy: Guided by MRI or CT scans, the surgeon drills a very small hole into the skull precisely over the location of the tumor. A very small, hollow needle then withdraws a small part of the tumor. This approach is usually used to biopsy tumors in areas where surgery may be difficult or dangerous, but a sample of tissue is still required for precise diagnosis.
- Craniotomy: If the surgical team believes that they can safely remove all or most of the tumor, a biopsy will be performed as the tumor is removed. Small samples of the tumor are examined immediately during the surgery to determine whether further surgery is required.
- Lumbar puncture (spinal tap): This test is used to determine whether there are cancerous cells in the cerebrospinal fluid, or the fluid that surrounds the brain and spinal cord. The test involves removing some of the fluid through a small needle inserted between the bones of the spine.
- Bone marrow aspiration and biopsy: This test may need to be done if it is believed the tumor has spread beyond the nervous system. During the aspiration, a small amount of liquid bone marrow is removed from a large bone, usually the hip bone, using a small, hollow needle. A biopsy involves removing a small piece of bone along with some of the marrow.
More about Childhood Brain Tumor Cancers:
- About Childhood Brain Tumor Cancer – Detection and Diagnosis
- Causes, Risk Factors, and Prevention of Childhood Brain Tumor Cancer
- What are the signs and symptoms of Childhood Brain Tumor Cancer?
- Childhood Brain Tumor Cancer Treatment
- Childhood Brain Tumor Cancer – Stages and Prognosis
- What is the expected life span of Childhood Brain Tumor Cancer?
- After Treatment – Living as a Childhood Brain Tumor Cancer Survivor
More about Childhood Spinal Cord Tumor Cancers:
- About Childhood Spinal Cord Tumor Cancer – Detection and Diagnosis
- Causes, Risk Factors, and Prevention of Childhood Spinal Cord Tumor Cancer
- What are the signs and symptoms of Childhood Spinal Cord Tumor Cancer?
- Spinal Cord Tumor Cancer Treatment
- Spinal Cord Tumor Cancer – Stages and Prognosis
- What is the expected life span of Childhood Spinal Cord Tumor Cancer?
- After Treatment – Living as a Childhood Spinal Cord Tumor Cancer Survivor
Learn More About the Different Types of Childhood Cancers:
- Childhood Brain Tumor Cancer (Brain Stem Tumors)
- Spinal Cord Tumor Cancer
- Childhood Neuroblastoma Cancers
- Childhood Hodgkin Lymphoma Cancers
- Non-Hodgkin Lymphoma Cancers
- Wilms tumor (Kidney Tumors)
- Rhabdomyosarcoma
- Retinoblastoma
- Bone cancer (including osteosarcoma and Ewing sarcoma)
- Leukemia Cancers: Acute lymphocytic (lymphoblastic) leukemia (ALL) Acute myelogenous leukemia (AML); Juvenile myelomonocytic leukemia (JMML)
- Hepatoblastoma (Liver Cancer)
- Rhabdoid Tumors
About American Childhood Cancer Organization
American Childhood Cancer Organization (ACCO) is a non-profit charity dedicated to helping kids with cancer and their families navigate the difficult journey from cancer diagnosis through survivorship. Internationally, ACCO is the sole U.S. member of Childhood Cancer International (CCI), the largest patient-support organization for childhood cancer in the world. Here in the United States, ACCO promotes the critical importance of ensuring continued funding into new and better treatment protocols for childhood cancer. And most importantly, ACCO is focused on the children: developing and providing educational tools for children fighting cancer and their families, empowering them in their understanding of childhood cancer and the medical decisions they must make during this difficult journey. All of ACCO’s resources are available free of charge for families coping with childhood cancer.
For additional information about childhood cancer or on the ACCO, or to order resources for you or your child, please visit our website at www.acco.org , call 855.858.2226 or visit:

