TREATING HIGH-RISK NEUROBLASTOMA AT THE TURN OF THE CENTURY
by C. Patrick Reynolds, MD PhD & Beth Hasenauer, RN MS Source: Spring 2001 CCCF Newsletter
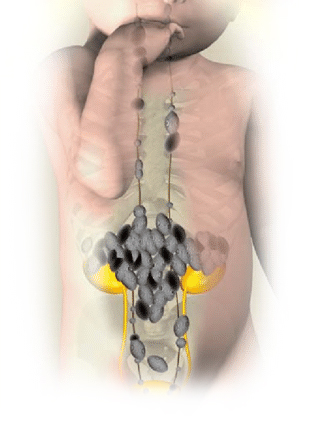 Neuroblastoma is a solid tumor of childhood that arises in the nervous system, outside of the brain. The goal of this article is to provide a guide to the initial treatment options available for children with high-risk neuroblastoma. Also reviewed, will be the design and conduct of clinical trials. This information will be of interest to parents dealing with other childhood cancers.
Neuroblastoma is a solid tumor of childhood that arises in the nervous system, outside of the brain. The goal of this article is to provide a guide to the initial treatment options available for children with high-risk neuroblastoma. Also reviewed, will be the design and conduct of clinical trials. This information will be of interest to parents dealing with other childhood cancers.
During the last part of the 20th century, clinical trials have shown that the basis for treating high-risk neuroblastoma should consist of induction chemotherapy, consolidation with high dose chemotherapy + stem cell transplant. The stem cell transplants use the patient’s own previously stored stem cells obtained from either the bone marrow or peripheral blood (PBSC) to replace the bone marrow, which is destroyed by the high-dose chemotherapy. Patients also receive local radiation to tumor sites, followed by posttransplant maintenance treatment with 13-cis-retinoic acid (Accutane). 13-cis-retinoic acid is aimed at eliminating any remaining tumor cells that are possibly left after the transplant. These established principles apply to “up-front” therapy of high-risk neuroblastoma.
To date, a single large clinical study with long-term survival data (the Childrens Cancer Group CCG-3891 study) has employed all of these therapeutic principles uniformly in a large group of patients beginning at diagnosis. Based on the CCG data, a child diagnosed with high-risk neuroblastoma when treated with the above approaches, can expect an estimated 40% probability of disease- free survival four years from diagnosis. Potential improvements in all components of therapy (induction chemotherapy, intensive consolidation with stem cell transplant, and post-transplant therapy) have occurred since the CCG-3891 study. Thus, it is reasonable to expect the potential for a higher disease- free survival for high-risk neuroblastoma in ongoing and future clinical trials.
For those patients in whom the tumor progressively grows during or after therapy, the chances of survival are reduced. Because there are no established effective treatments for such patients, therapies listed above and/or highly experimental therapies with unknown risks may be appropriate for such patients.
WHAT IS HIGH-RISK NEUROBLASTOMA?
The clinical behavior of neuroblastoma is highly variable, with some tumors being easily treatable, but the majority being very aggressive. This article will only address therapy of high-risk neuroblastoma. The treatment of low or intermediate risk tumors is very different from treating high-risk disease. All patients with stage 4 disease diagnosed after one year of age are classified in the high-risk category. In stage 4 disease, the neuroblastoma tumor cells have already spread (or metastasized) to other sites in the body, such as the bone or bone marrow. Essentially all patients who have tumors with many copies (or amplification) of the MYCN oncogene also have high-risk disease, even if they do not have evidence of the tumor having spread. Given the aggressiveness of the tumor type, it is accepted practice to treat high-risk neuroblastoma patients with intensive therapy, to increase the probability of cure. Most pediatric oncologists agree that even with optimal current intensive therapy, the aggressive nature of this disease warrants entering as many of these children as possible on clinical trials that may identify improved forms of treatment.
CLINICAL TRIALS
Clinical trials are research studies that test a new approach to therapy. Phase III clinical trials focus on a particular disease and ask specific scientific questions, with the long-term goal of defining the best approach to treatment by comparing one therapy to another. These large studies test a new treatment/ procedure in comparison to the current standard treatment by using randomized assignment to determine which of these approaches offer an improvement in terms of outcome and patient safety as compared to the current standard. Those patients who cannot participate in a clinical trial should receive therapy that has been proven in previous clinical trials to be safe and to deliver the best-proven probability of achieving long-term survival.
An advantage to participating in a clinical trial is that the patient receives a therapeutic approach that has been mapped out and reviewed by a team of investigators who specialize in the disease being studied.
Participation in clinical trials allows patients access to state-of-the-art treatment for that disease and also the chance of being among the first to benefit from a new treatment that may be more effective.
All clinical trials are reviewed by the committee for protection of human subjects (also known as Institutional Review Board or IRB), at the institution where the patient is treated. This review ensures that the rights of the patient will be upheld and protected and that the patient will not be exposed to any unnecessary or extreme risk if he/she agrees to participate in the clinical trial.
The larger the organization carrying out the trial, the greater the review of the plan of therapy. For example, a phase III cooperative group trial (in pediatric oncology, a nationwide trial) would be reviewed by many pediatric oncologists, surgeons, pathologists, radiation oncologists, nurses, statisticians, etc in the cooperative group, by the National Cancer Institute’s Cancer Treatment Evaluation Program (CTEP), and by the IRB’s of many dozens of institutions.
There are currently several different clinical trials in the United States for newly diagnosed high-risk neuroblastoma. Most of the these trials utilize initial therapy (induction chemotherapy and perhaps surgery), followed by high-dose chemotherapy with stem cell transplant using the patient’s own stem cells. Most studies also employ local radiation, and after completion of all cytotoxic therapy (including stem cell transplant and radiation), Accutane is given for six months. Phase III trials conducted by the national cooperative group (The Childrens Oncology Group, or COG) occur without change over more then 3 years, so we will review those trials in detail. Table 1 summarizes most of the modalities of therapy currently being tested in clinical trials for high risk neuroblastoma, including phase I and phase II studies.
CHILDRENS ONCOLOGY GROUP (COG) PHASE III STUDIES
The Childrens Oncology Group is a national group of physicians, nurses, and other specialists devoted to the study of childhood cancer. Phase III trials run by cooperative groups such as the COG help to establish state of the art cancer therapy. There are currently 2 planned COG phase III trials for high-risk neuroblastoma. Both of these trials will enroll the same group of patients because the treatments being tested are sequential in nature. This means that a patient enrolled on the first study (known as A3973) may, but is not required to, enroll on the study that comes later in therapy, which is known as ANBL0032. However, patients who do not enroll on the A3973 study beginning at diagnosis are not eligible to participate in the ANBL0032 study. This requirement is to insure the statistical validity of the studies.
The A3973 study, which opened on February 10, 2001 employs very aggressive multi-drug induction chemotherapy, during which patient’s PBSC are harvested, ideally after 2 cycles of chemotherapy. The major research question being asked in this study is: Does selective removal (purging) of tumor cells from PBSC improve the tumor-free survival of patients given a stem cell transplant? To address this question, half of the patients are randomized to have their stem cells treated with antibodies attached to magnetic beads, which are then used to remove any residual tumor cells that might be remaining in the PBSC. The other half have their untreated stem cells stored for subsequent use. After successfully storing purged or un-purged PBSC, patients will complete 4 additional cycles of chemotherapy (for a total of 6 cycles), followed by intensive myeloablative chemotherapy and the PBSC reinfusion. The myeloablative therapy used in A3973 is known as CEM-LI (carobplatin, etoposide, melphalan, local irradiation). Patients receive the local radiation after the stem cell transplant to the primary tumor site and other sites of known metastases, followed by 6 months of Accutane. Patients on A3973 are eligible to enter the ANBL0032 study.
The ANBL0032 study is testing a monoclonal antibody (ch14.18) that attaches to neuroblastoma cells which have a molecule called GD2 on their surface. Once the antibody attaches to the GD2 it helps the tumor cells to be destroyed. This antibody does not attach to most normal cells because they do not have GD2 on their surface. Laboratory experiments and small clinical trials suggest that ch14.18 can help the body’s own immune cells to destroy neuroblastoma cells. These immune cells include cells that are activated by GM-CSF (monocytes and neutrophils) and cells that are activated by IL-2 (lymphocytes). The antibody ch14.18 + GM-CSF or IL-2 will be given after completion of intensive therapy supported by PBSC infusion (A3973 therapy). In addition, 13-cis-retinoic acid (Accutane) will also be given in between cycles of therapy with ch14.18 + GM-CSF or IL-2. The purpose of giving antibody therapy and 13-cis-retinoic acid is to maximize the chances of eliminating any residual neuroblastoma tumor cells (known as minimal residual disease) that may be left after intensive therapy, such as that given in A3973.
Recurrent or Progressive Neuroblastoma: High-risk neuroblastoma patients who develop progressively growing tumors during therapy, or have tumor recurrence after chemotherapy, are encouraged to enter into phase I or II clinical trials that test new approaches to therapy. Some of these studies are carried out within the COG, some within a multi-institutional consortium funded by the National Cancer Institute known as the New Approaches to Neuroblastoma Therapy (NANT) Consortium, and some within individual institutions. Examples of such studies are included in Table 1 below. Because the toxicity (especially the long term toxicities) of these new therapies are not fully known, and because the ability of these therapies to improve outcome for patients is not proven, many of these new approaches are limited to testing in patients with recurrent disease.
MODALITIES OF THERAPY CURRENTLY IN CLINICAL TRIALS FOR HIGH-RISK NEUROBLASTOMA
Induction chemotherapy. Chemotherapy that doesn’t require marrow or PBSC support. Examples of drugs used include cyclophosphamide, cisplatin, carboplatin, vincristine, doxorubicin, etoposide, ifosfamide, and topotecan.
Surgery: Partial or total surgical removal of the tumor.
Local Radiation: Radiation given to a localized area that includes the tumor.
Myeloablative Therapy: Very intensive chemotherapy or chemotherapy + total body irradiation that destroys the marrow cells, requiring the infusion of marrow or PBSC to restore marrow function. Myeloablative therapy approaches currently being tested include those with intensive chemotherapy, those with intensive chemotherapy + local irradiation, and multiple rounds of myeloablative therapy (tandem transplants).
Antibody Therapy: Administration of a monoclonal antibody that attaches to tumor cells, of ten together with factors called cytokines that stimulate white blood cells (attached to the tumor via the antibody) to kill the tumor cell. Examples of antibody therapy include the ch14.18 antibody, the 3F8 antibody, and a new designer molecule (called an immunocytokine) in which the hu14.18 antibody (an anti-GD2-antibody) is fused together with the IL-2 cytokine.
Retinoid Therapy: Administration of high doses of a drug that is derived from vitamin- ”A”, which has an anti-tumor effect. Retinoids usually have very little or no marrow cytotoxicity and so they are employed soon after myeloablative therapy. Accutane (13- cis-retinoic acid) is a retinoid that causes the neuroblastoma cells to stop growing and differentiate (mature) into more normal appearing cells. Fenretinide is a newer retinoid that, rather then inducing tumor cell differentiation, kills neuroblastoma cells.
MIBG: Administration of high doses of a radioactive chemical selectively taken up by neuroblastoma cells. The MIBG molecule is made with radioactive iodine (131I), which is why the thyroid has to be protected during such therapy. The concentration of the MIBG at the tumor results from the tumor pulling in the MIBG, concentrating the radiation into the tumor. This provides very high doses of radiation to the tumor cells.
Vaccine Therapy: Injection of substances into patients that are designed to stimulate the immunological system to attack the tumor. Examples of such vaccines include tumor cells that have been engineered to make cytokines (those molecules that stimulate the immune system) or antibodies that are designed to elicit an antibody response that will attack the tumor. Antibodies produced by the patient in response to the vaccine could be effective in attacking neuroblastoma cells. Such antibodies are known as “anti-idiotypic antibodies”. Another approach being tested involves genetically engineering neuroblastoma cells so that the tumor cells make a cytokine, irradiating those cells to prevent them from forming tumors, and injecting those cells into the patient to stimulate the immune system.
RESOURCES FOR FURTHER INFORMATION
The internet provides a medium for rapid exchange of information. The following are just some of the information resources available to parents of children with neuroblastoma on “the net”:
The NBLASTOMA mailing list is an automated email mailing list where parents of children with neuroblastoma can communicate with one another. In addition to being able to join the list, one can find the archives of the list (which contains a lot of information and discussion in previous posts to the list). The list web site is: listserv.acor.org/archives/n-blastoma.html (http://listserv.acor.org/SCRIPTS/WA-ACOR.EXE?A0=N-BLASTOMA)
National Cancer Institute (NCI) site devoted to cancer clinical trials: www.cancer.gov/clinicaltrials
The COG web site: www.curesearch.org
The New Approaches to Neuroblastoma Therapy (NANT) web site: www.nant.org
Acknowledgements. The authors thank Dr. Robert Seeger and Dr. Clarke Anderson of Childrens Hospital Los Angeles for helpful review of, and suggestions concerning, this article.
ACCO would like to thank Dr. Patrick Reynolds, MD PhD and Beth Hasenauer, RN MS, of Children’s Hospital Los Angeles for their on-going commitment towards the improved care of children with neuroblastoma and the writing of this invaluable article.
More about Childhood Neuroblastoma Cancers:
- About Childhood Neuroblastoma Cancer – Detection and Diagnosis
- Causes, Risk Factors, and Prevention of Childhood Neuroblastoma Cancer
- What are the signs and symptoms of Childhood Neuroblastoma Cancer?
- Childhood Neuroblastoma Cancer Treatment
- Childhood Neuroblastoma Cancer – Stages and Prognosis
- What is the expected life span of Childhood Neuroblastoma Cancer?
- After Treatment – Living as a Childhood Neuroblastoma Cancer Survivor


