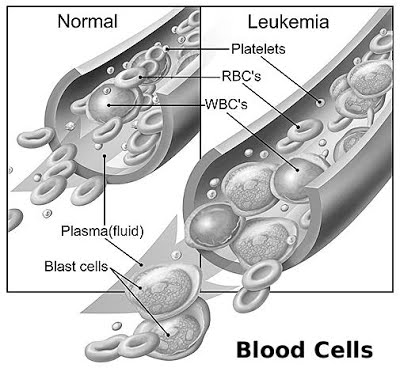
What is the Treatment for Childhood Leukemia?
The majority of children diagnosed with childhood leukemia will be treated with chemotherapy. Chemotherapy (often simply called “chemo” for short) involves targeting cancerous cells with specific drugs. The specific type of drugs, their dosages, and the duration of the treatment will be unique to each patient, depending on the type and classification of leukemia, the cancer’s classification of risk, and the specific needs of each child. Surgery and radiation are not commonly utilized in the treatment of childhood leukemia, although they may be required to address specific health issues in certain cases. Because chemotherapy can have significant short- and long-term health effects on childhood leukemia survivors, researchers are continuing to investigate new and less toxic treatments such as immunotherapy and targeted chemotherapy; however, these treatments are still in the research phase.
Because AML and ALL are the two most common types of childhood leukemia, this discussion will focus specifically on their treatment.
Chemotherapy for ALL
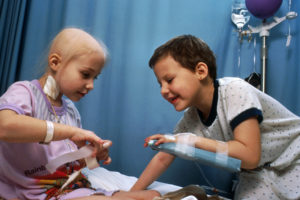 Treatment for children with Acute lymphocytic leukemia (ALL) usually involves smaller dosages of chemotherapy but spread over a period of two-to-three years (boys often receive treatment for longer than girls, due to a higher risk of recurrence). For most children with ALL, chemotherapy will involve three distinct phases:
Treatment for children with Acute lymphocytic leukemia (ALL) usually involves smaller dosages of chemotherapy but spread over a period of two-to-three years (boys often receive treatment for longer than girls, due to a higher risk of recurrence). For most children with ALL, chemotherapy will involve three distinct phases:
- Induction: The goal of induction is to kill 99% of existing cancer cells and achieve “remission”, in which no cancer cells are found in the bone marrow and blood counts return to normal (this is not, however, the same as a “cure”). Induction usually lasts about one month and is extremely intense, requiring prolonged hospital stays and frequent visits to the doctor. Induction almost always includes intrathecal chemotherapy, in which the chemotherapy is targeted at the cerebrospinal fluid to kill any cancer cells that may have spread to the brain and/or spinal column.
- Consolidation (intensification): This phase usually lasts for 1-2 months and is designed to reduce the number of cancer cells remaining in the body, as well as fight the potential for drug resistance among those cancer cells. This phase is also highly intense (often more so than induction).
- Maintenance: About 95% of children with ALL will achieve remission after induction and consolidation. For these children, an additional 2 years of so-called maintenance chemotherapy will help prevent the disease from recurring. Maintenance is much less intensive, and usually involves the administration of chemotherapy for brief periods every 4-8 weeks. The early part of maintenance may involve 1-2 months of intensified treatments called re-induction or delayed intensification.
Chemotherapy for AML
Chemotherapy for AML is more intensive, involving higher dosages of treatment drugs but over a shorter duration. Chemotherapy for AML includes an induction phase and a consolidation (intensification) phase, but usually lacks a maintenance phase.
- Induction: Induction for AML usually involves the administration of drugs for several days in a row, with treatments scheduled every 10-14 days. Less time between treatments is generally more effective but can lead to more severe side effects. Each treatment plan will depend on the child’s unique disease progression and their reaction to the chemotherapy. Treatment will continue until the bone marrow is clear of leukemia cells, usually after 2-3 treatment cycles. As with ALL, treatment usually involves intrathecal chemotherapy as well.
- Consolidation (intensification): Between 85-90% of children with AML will achieve remission after the induction phase. Consolidation usually involves several more months of intensive chemotherapy, as well as intrathecal chemotherapy. In some cases, a stem cell transplant from a sibling may be appropriate as well, especially for children with high risk AML.
Although the duration of treatment is shorter for AML, it requires extensive supportive care and attention to ancillary issues such as nutrition, medication, and blood transfusions to cope with the more severe side effects, including (but not limited to) damage to the bone marrow responsible for creating new blood cells.
More about Childhood Leukemia Cancers:
- About Childhood Leukemia Cancer – Detection and Diagnosis
- Causes, Risk Factors, and Prevention of Childhood Leukemia Cancer
- What are the signs and symptoms of Childhood Leukemia Cancer?
- Childhood Leukemia Cancer Treatment
- What is the expected life span of Childhood Leukemia Cancer?
- After Treatment – Living as a Childhood Leukemia Cancer Survivor
Learn More About the Different Types of Childhood Cancers:
- Childhood Brain Tumor Cancer (Brain Stem Tumors)
- Spinal Cord Tumor Cancer
- Childhood Neuroblastoma Cancers
- Childhood Hodgkin Lymphoma Cancers
- Non-Hodgkin Lymphoma Cancers
- Wilms tumor (Kidney Tumors)
- Rhabdomyosarcoma
- Retinoblastoma
- Bone cancer (including osteosarcoma and Ewing sarcoma)
- Leukemia Cancers: Acute lymphocytic (lymphoblastic) leukemia (ALL) Acute myelogenous leukemia (AML); Juvenile myelomonocytic leukemia (JMML)
- Hepatoblastoma (Liver Cancer)
- Rhabdoid Tumors
About American Childhood Cancer Organization
American Childhood Cancer Organization (ACCO) is a non-profit charity dedicated to helping kids with cancer and their families navigate the difficult journey from cancer diagnosis through survivorship. Internationally, ACCO is the sole U.S. member of Childhood Cancer International (CCI), the largest patient-support organization for childhood cancer in the world. Here in the United States, ACCO promotes the critical importance of ensuring continued funding into new and better treatment protocols for childhood cancer. And most importantly, ACCO is focused on the children: developing and providing educational tools for children fighting cancer and their families, empowering them in their understanding of childhood cancer and the medical decisions they must make during this difficult journey. All of ACCO’s resources are available free of charge for families coping with childhood cancer.
For additional information about childhood cancer or on the ACCO, or to order resources for you or your child, please visit our website at www.acco.org , call 855.858.2226 or visit: